The human body is a haven for life. It is much like a prosperous country prone to attack throughout the entire life. Every minute of every day, trillions of the tiniest cells are working all the time to help keep our body healthy. Our amazing immune system knows just what to do. However, it is something we probably do not think about until something goes wrong. That’s what happens with an autoimmune disorder.
In this article, let’s take a walk through autoimmune disorder.
READ ALSO: The ABCs of Hepatitis
Self-protection system
Our immune system can recognise and tolerate the healthy cells in our body. In order words, the immunity army of our body – the white blood cells – do not attack the healthy cells of our body.
Why does that happen?
Every healthy cell in our body has its own self-ID called “self-antigen”. This self-ID enables the patrolling immune cells to recognise them as self-proteins7.
Therefore, under normal condition, our immune system will have no problem distinguishing between healthy cells and violating pathogens.

Autoimmunity
In specific individuals, the immune system might lose its ability to recognise and tolerate the body healthy cells. As a result, the immune system will take the healthy cells as violating pathogens and start attacking them without any mercy. This condition is called autoimmunity or autoimmune disorder.
Example of Autoimmune Disorder
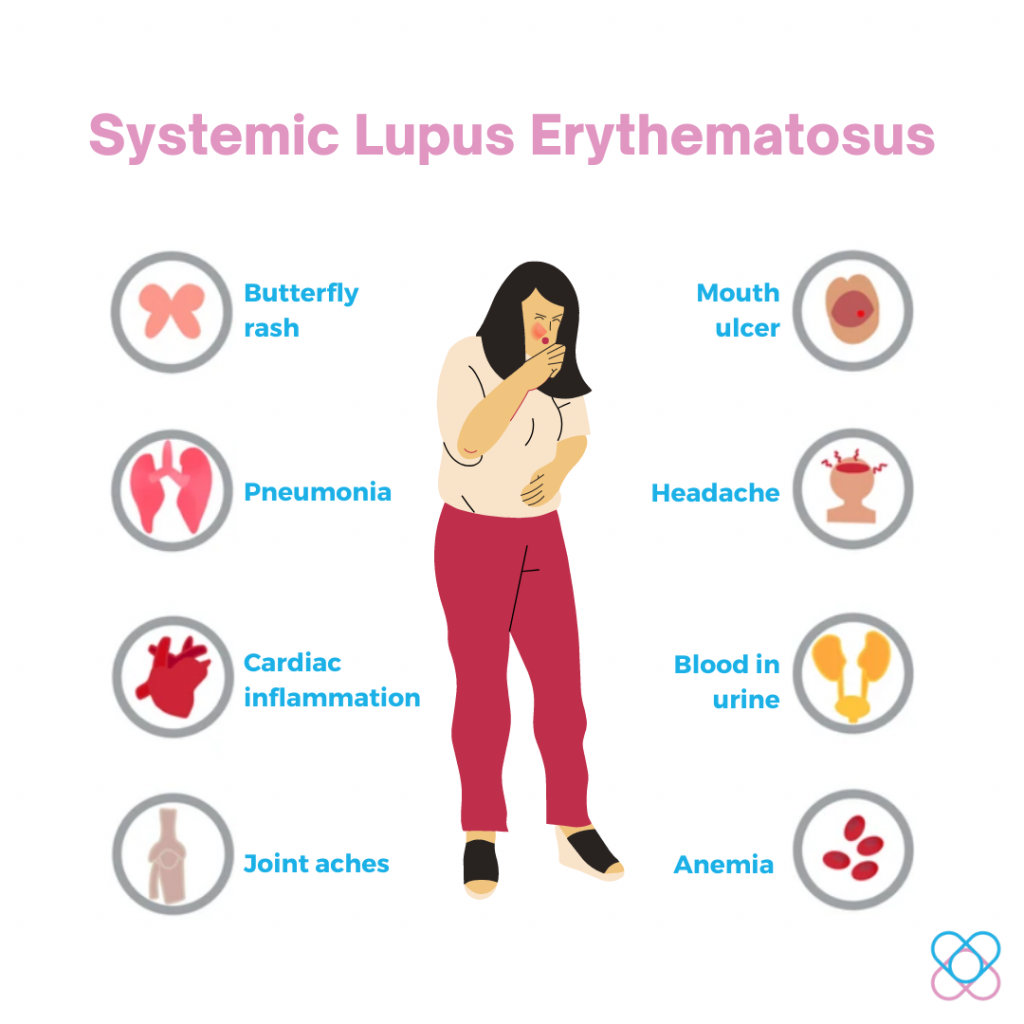
Systemic Lupus Erythematosus (SLE)
SLE is a severe multisystem autoimmune disorder. Almost any organ or system within the body can be affected; lupus is the classical multi-symptom illness. In this case, the immune system produces antibodies directed against self-antigens, causing local inflammation and organ damage2.
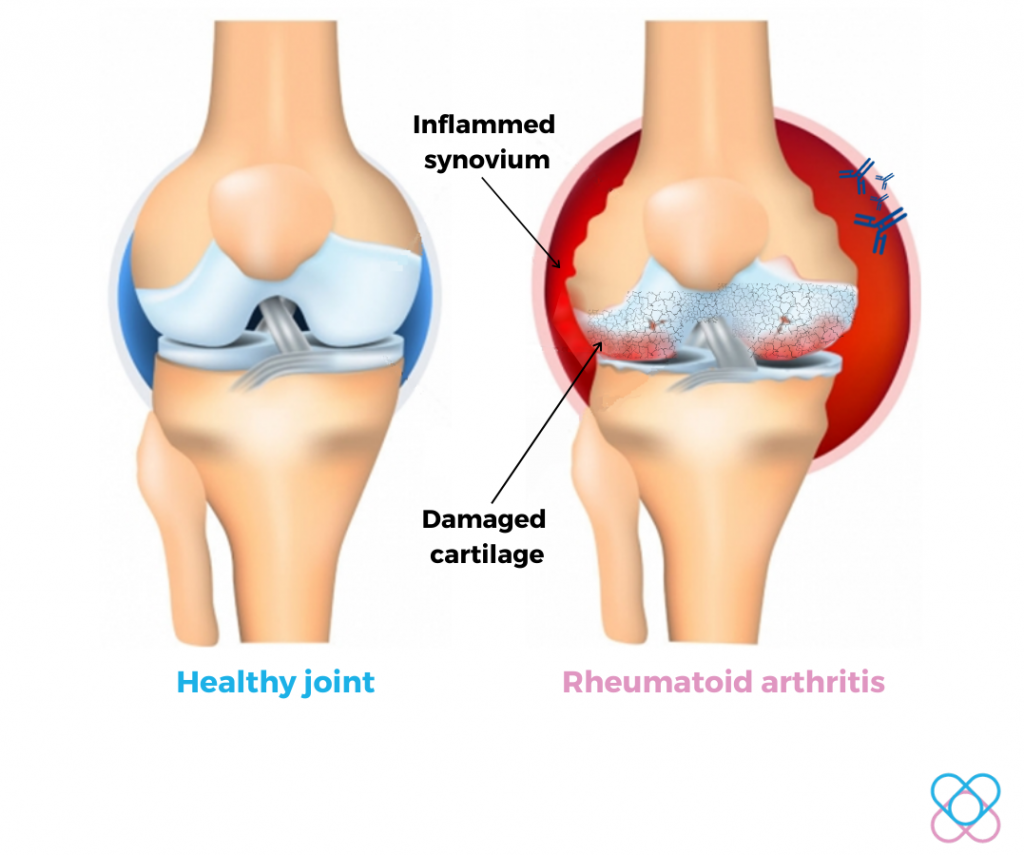
Rheumatoid Arthritis
The immune system produces antibodies that attack the smooth lining of a joint (synovium). This causes inflammation and pain in the synovium5. If left untreated, it can potentially damage the cushion between bones (cartilage) and distort the joint.
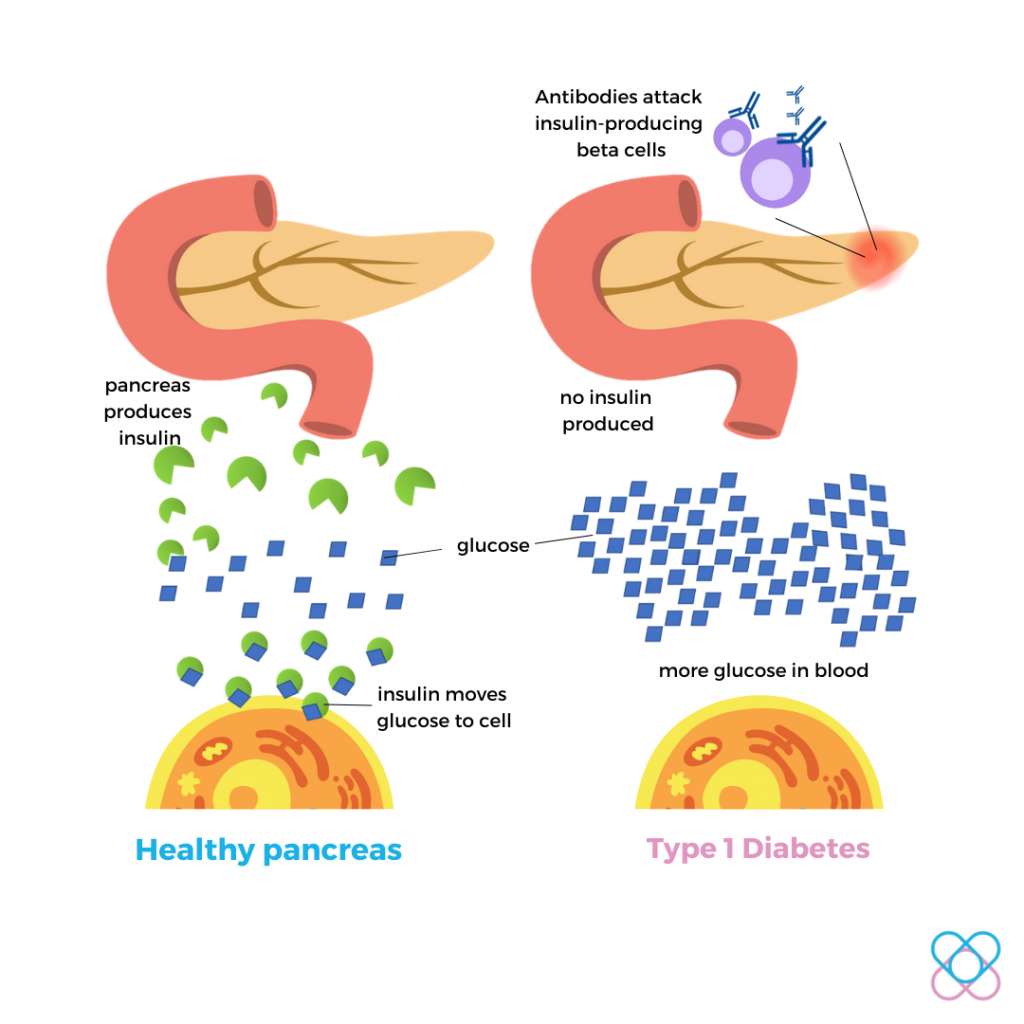
Type 1 Diabetes
The immune system sends antibodies to the pancreas to attack the insulin-producing (beta) cells.
Risk Factors
Although this topic is heavily researched, we still do not fully understand the exact trigger for an autoimmune response.
Some possibilities include genetic mutations, infection by pathogens and damage to immunologically privileged tissue.
Genetic mutation
A genetic mutation is believed to be one of the possible causes of developing autoimmune disorder6. Healthy cells display self-antigen (self-ID) on a membrane-bound protein called “major histocompatibility complex” (MHC). This complex acts like a SIM on the self-ID card that gives the real “self” identity to the healthy cells. This SIM together with the self-ID card mediates the self-recognition process by the white blood cells.
Genetic mutations of DNA that code for the MHC may lead to the failure of self-recognition by immune cells. In other words, the mutated cell no longer has the ability to display a self-ID card with intact SIM. The immune system cannot verify the damaged SIM and will recognise the cell as foreign and start to get rid of it.
Pathogenic infection
During pathogen infection, the invading pathogens may contain or produce antigens (ID card) that resemble the self-ID of the healthy body cells1. When the pathogenic infection triggers the immune response, the antibodies produced may then attack both the healthy cells and pathogens.

Immuno Privileged Sites
Certain sites of the body are not accessible by immune cells due to the absence of conducting blood and lymph vessels.
Physical damages to these “privileged” sites will release self-antigens (ID card) that the immune system has not yet encountered. Therefore, the white blood cells will recognise the ID as “foreign”, self-attacking the damaged “privileged” tissue and triggering an autoimmune response that can destroy those areas3. The cornea, testes, and brain are the example of these fragile privileged sites.

Bottom Line
There are more than 80 different autoimmune diseases that exist. Their triggered symptoms often overlap, making them hard to get an accurate diagnosis.
Autoimmune disorders are more common in women. They often run in families and may be passed down to the next generation4. A genetic test or biochemical blood test can help one diagnose these conditions and take appropriate treatment to calm down the overactive immune response in the body.
Worried if you are at risk of getting Systemic lupus erythematosus (SLE)? Find out more about your health risk in SLE with DNA Explorer today!
References
1. Christen, U. (2019). Pathogen infection and autoimmune disease. Clinical and experimental immunology, 195(1), 10.
2. Fairhurst, A. M., Wandstrat, A. E., & Wakeland, E. K. (2006). Systemic lupus erythematosus: multiple immunological phenotypes in complex genetic disease. Advances in immunology, 92, 1-69.
3. Forrester, J. V., Xu, H., Lambe, T., & Cornall, R. (2008). Immune privilege or privileged immunity?. Mucosal immunology, 1(5), 372-381.
4. Marrack, P., Kappler, J., & Kotzin, B. L. (2001). Autoimmune disease: why and where it occurs. Nature medicine, 7(8), 899-905.
5. Ménard, H. A., Lapointe, E., Rochdi, M. D., & Zhou, Z. J. (2000). Insights into rheumatoid arthritis derived from the Sa immune system. Arthritis Research & Therapy, 2(6), 1-4.
6. Ridgway, W. M., Fassò, M., & Fathman, G. C. (1999). A new look at MHC and autoimmune disease. Science, 284(5415), 749-751.
7. Sakaguchi, S., Powrie, F., & Ransohoff, R. M. (2012). Re-establishing immunological self-tolerance in autoimmune disease. Nature medicine, 18(1), 54-58.

